The role of inclusive research in tackling inequalities and promoting fresh thinking
Savitri Hensman, involvement coordinator at ARC South London, explores the real-world consequences of inadequate inclusion in research.
Savitri Hensman, involvement coordinator at ARC South London, explores the real-world consequences of inadequate inclusion in research.
The importance of “research inclusion” – or sometimes “equity [or equality], diversity and inclusion” (EDI) in research – is now nationally as well as locally recognised. This is largely in response to concerns among patients, carers and communities, as well as researchers, care and health workers, that there are still high levels of suffering and early death which could have been prevented. In addition, more people realise that it is unfair, and a loss to research, when people who could have added much to knowledge as senior researchers are blocked because of an aspect of their identity.
In December 2024, National Institute of Health and Care Research (NIHR) leaders explained why more inclusive research was now a funding condition. They flagged up the alarming example of a widely-used medical device which might fail to detect dangerously low levels of blood oxygen in a sizeable part of the population. This includes numerous South Londoners – and even those not at direct risk often have family or friends who are.
While publicity has sometimes focused on improving care and prevention for minorities, women and those who are both, which is important indeed, the scope is far wider. Almost everyone may benefit in some way from greater focus on inclusive approaches which reduce inequalities and allow all to thrive.
Much fresh thinking is underway in this field, opening the door to scientific as well as practical advances. But I also think there are areas in which confusion is widespread; and challenges, as well as opportunities, persist, including in involvement. It is important to encourage and support a wide range of people to be actively involved, along with recruiting and gathering data from diverse participants and being respectful and considerate. But more still is needed.
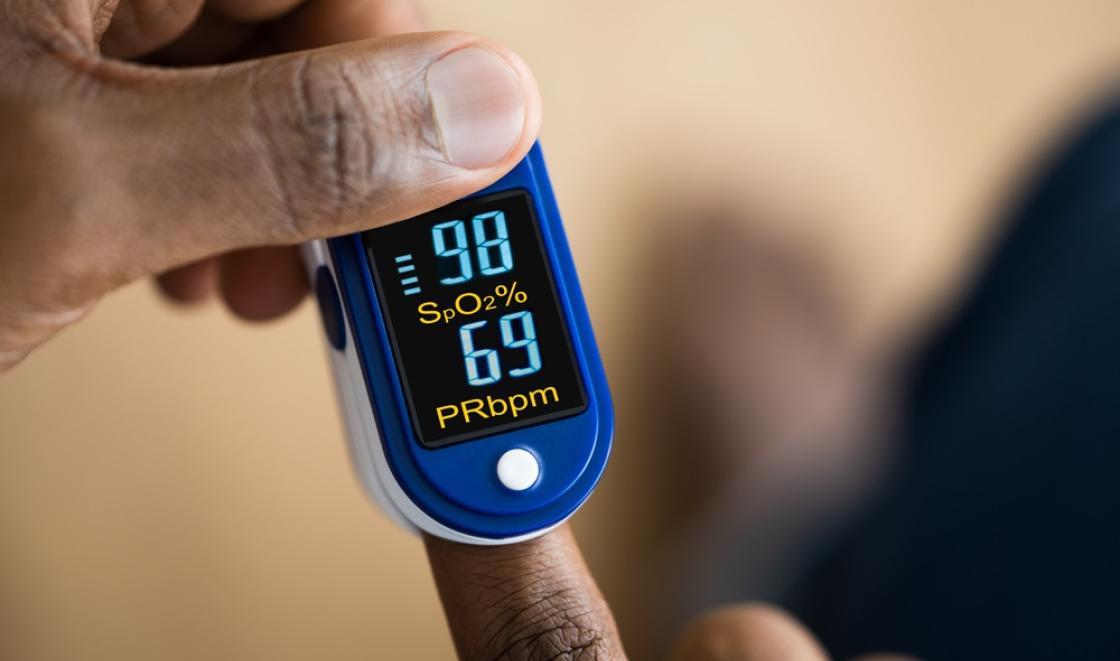
Examples given by NIHR (including in a video) of why research inclusion should be strengthened include cases where the samples studied were quite different from those actually likely to use the treatment and that of pulse oximeters. These are often clipped to someone’s finger to check their blood oxygen level but may be inaccurate if they have dark skin.
For decades, it has been known that those on whom medication or equipment is tested may not reflect the varied people who go on to use it. Efforts have been made to change this but there is still quite a way to go. At one time, researchers often relied on results based on adults of working age, mainly men and those without multiple conditions. Sometimes these participants were almost all white (unless lower costs and maybe fewer safety restrictions made it more attractive to carry out drug trials in the global South, or minorities were selected for ethically flawed research).
Then these results might be assumed to apply to adults of any gender or ethnic group, even if, in reality, treatments might be less effective or safe for some than others. If children were treated, what was prescribed might be based on guesswork, for instance, that they be administered half the adult dose, or a proportion based on body weight.
For adults with multiple conditions (often older), health professionals might go by published findings based on studies on a different set of people with less chance of complications, or their own rather different clinical experience, and again hope for the best. Other types of health research too were often based on whom it was easiest to recruit, especially if approaches other than randomised trials were undervalued. Meanwhile social care research sometimes glossed over the problem that many service users missed out on freedoms which others enjoyed.
It became increasingly clear that the research world needed to do better, largely because people with lived experience were taking action and increasingly carrying out research themselves. Others who cared about justice also took up concerns. Human diversity and the needs, experiences and views of people facing economic hardship and/or discrimination were more often taken on board and sometimes became central to research, though gaps remained.
It can be easier to get funding and publicity by “proving” how successful something is than by pointing out when, and for whom, it might not work, or exploring research ideas developed by under-served groups.
Approaches such as the ‘King’s Model’ showed how focused effort and building trust could greatly boost participation, and indeed involvement, among minority ethnic people, so that those studied more closely reflected a diverse population. Yet the problem with oximeters shows this is not enough.
Methods may be required which can identify whether a medicine, activity or factor in the environment affects people differently depending on ethnicity, age, class and so forth; or shed light on varied experiences of services or risks. This offers challenges in both qualitative and quantitative study design.
Giving people with lived experience a real say – especially if equal partners or lead researchers – can advance equity in who shapes and conducts research, what is studied and how and the use made of findings. To start with, often those researched might count as disabled people in UK law, while researchers are mainly not. Or the focus may be on communities at risk or experiencing gaps because they are marginalised in some way, but who have little input.
At the same time, patients, carers and members of the wider public, like researchers and health and care professionals, may absorb widespread prejudices or mistaken assumptions about certain groups, even their own. There are differences in power, status and views within communities, as well as between researchers and participants or people involved. I believe public contributors and lived experience researchers, alongside everyone else, should be encouraged to think and learn about research inclusion.
This does not mean having to be experts in every type of methodology or inequity – hardly anyone is! But awareness matters, including openness to reflecting on self and society. And, for people interested in this rapidly-developing field, there are now more resources which non-specialists might understand.
Even if diverse people are actively involved, research culture and funding may lead to focusing just on cultural issues or personal or community behaviours which affect wellbeing, rather than inequity. Or inequalities may be seen as solely stemming from discriminatory behaviour by individual health and care professionals or managers. These are important. Yet systems too can damage health, and not only by failing to pick up on staff prejudice.
Disentangling the multiple ways in which inequity can affect a set of people can be a challenge, including for people with lived experience. This can be a valuable source of insight and driver for change. Yet it may be tempting to focus on factors we have experienced or observed which most affected us, when others too may influence what happens. And recalling inequity can be draining as well as energising. Space to explore possibilities and feelings can be valuable.
Other challenges include a backlash in parts of the world against EDI (sometimes known as DEI). This is hitting the USA, badly affecting health research and care not only for minorities but also lower-income rural and sometimes urban white Americans. Resisting this trend may require promoting understanding of what EDI is and its benefits. This includes avoiding approaches which encourage feeling guilty rather than taking action; or using everyday words to mean something very different, confusing all but the highly-educated in that field.
More subtly, there may be a push for policies which are likely to increase health inequity. For instance, research evidence indicates that cutting social security for disabled people causes harm and does not encourage them into employment. While research organisations can feel pressure to stay quiet, this is a chance for researchers, people with lived experience and communities together to demonstrate why research is so important, showing which “solutions” make matters worse.
Research inclusion, with diverse involvement, is not always easy, yet brings many benefits.
Read about the patient and public involvement work being carried out at ARC South London.